Patients drawn to new magnetic depression treatment
Depression, a common condition long relegated to the shadows, may be having its day in the sun.
“There’s still a stigma in talking about depression, but I think there is a start of a #metoo moment going on for mental health,” said Dr. Manish Sheth, medical director for San Diego-based Achieve TMS, a depression treatment center which recently opened a location in Claremont. “Before, it was something that was completely hush-hush, but that is changing.”
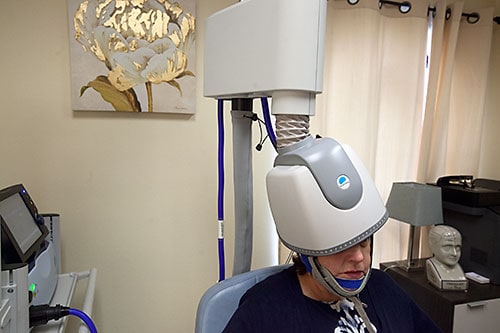
The 48-year-old doctor is at the forefront of a relatively new treatment for the disorder. Transcranial magnetic stimulation, or TMS, is a noninvasive technique that involves a coil that sits on a user’s head and applies repeated magnetic pulses the underlying limbic system or mood center of the brain.
“It stimulates the parts of the brain which are involved with depression,” Dr. Sheth said. “It also increases blood flow, changes the network speed in the brain, and alleviates depression.”
Treatments are comprised of about 36 sessions over nine weeks. The procedure is new, but the technology has been around for 20 years, and has been FDA approved for treating severe depression since 2008.
According to latest figures available from the National Institute of Mental Health (a branch of the National Institute of Health), an estimated 16.2 million adults in the United States had at least one major depressive episode during 2016, representing 6.7 percent of all US residents 18 or older. Among young people, an estimated 3.1 million adolescents aged 12 to 17 reported the same problem, representing a whopping 12.8 percent of the country’s population in that group. Females are much more likely to suffer in both groups, with the sexes splitting 8.5 women to 4.8 percent male among adults, and 19.4 to 6.4 among adolescents.
At present, TMS is FDA approved for patients ages 22 and older. However, several recent studies at Minnesota’s Mayo Clinic and other institutions have found it safe and effective for adolescents, Dr. Sheth said.
Traditionally, depression has been treated with talk therapy and medications such as Zoloft, Abilify, Prozac and dozens more. Like most medical treatments, results vary, and not everyone gets better. The FDA recommends patients have at least one medication failure before attempting TMS, Dr. Sheth said, and most insurance companies require at least two or more before they will authorize the treatment.
Of the patients who have failed with two or more medications, their chance of success with additional meds is somewhere around 15 percent. “But when they get TMS, they have a chance of response up to 80 percent of the time. It works as an augmentation.”
Dr. Sheth’s data comes from some 500 in-house questionnaires patients have completed at the end of each week of treatment. These are designed to determine how their levels of depression, anxiety and quality of life are changing, or not. “It’s one thing to look at their depression score, but we want to know if they’re feeling better,” Dr. Sheth said.
This data shows a post treatment result of “remission”—where depression symptoms had been reduced by 90 percent or more—in half of his patients.
Of the remaining respondents in the Achieve TMS survey, a “positive response”—meaning symptoms of depression were reduced by 50 percent or more—was reported 70 to 80 percent of the time.
Overall, about 20 percent of patients were less than 50 percent better after TMS, and 5 to 10 percent saw no improvement whatsoever.
Other studies have shown less striking results. A report published in 2011 by The World Journal of Biological Psychiatry showed a response rate of 63 percent and remission rate of 53 percent after 22 weeks of treatment along with medication trials. And, a 2010 NIMH study indicated much lower rates of remission—about 14 percent—from an initial round of TMS treatments, but that number climbed to 30 percent after a second series.
There is a reason for the disconnect in the numbers, Dr. Sheth said. “What is happening is that they are improving the systems by making it more precise and as we learn more you would see that the newer data shows even higher efficacy with the treatment.”
Additionally, Achieve TMS’s results are far better on a percentage basis than those seen with patients who only take medication and/or see a therapist, the doctor said. “It’s a huge number, because when you look at [just] medication, the response and remission rates are under 20 percent. With TMS, we don’t see anyone get worse. That is the best part. There is very limited, if any, downside.”
Another major benefit, Dr. Sheth says, is that oftentimes after TMS treatment, patients who had been on four or five antidepressant medications are usually able to cut that down to just one.
“It’s one thing to be not depressed, but then another to be feeling better. They are two different things. We look at things like, are they able to function at a higher level, are their relationships more meaningful, and are they better able to focus on their work, and what they do for leisure?”
There are precautions and there can be some negative side effects. Since magnets are being used, patients with steel in their brains due to previous surgeries cannot use the procedure. Most brain surgeries done over the past 20 years have involved titanium, which is safe for use with TMS. The most common side effects, affecting about 20 percent of patients, are headaches during in the first week of treatment. For most, these abate after about a week using over-the-counter headache meds.
Finally, the treatment carries with it a very small risk of seizure, Dr. Sheth said. In order to minimize this risk, TMS patients are screened prior to treatment for both caffeine and alcohol, which can increase the possibility of seizures. Those with a history of seizures, such as epileptics, can still receive the treatment, as long as they are stable and are not having daily events.
Dr. Sheth had planned on a more standard path in medicine. All that changed when he was a young medical student at South Gujarat University, in his homeland of India. “Depression has been kind of personal for me,” he said. “When I was in my four years of medical school, which can be stressful for many of us, I had three of my classmates commit suicide. When I saw that, I knew that I wanted to do something in this field. I couldn’t think of it as a collateral damage kind of thing. This was serious stuff.”
After graduation in 1993, he came to America to study at the University of South Dakota, earning a PhD in philosophy in 1999, and completing his residency in adult psychiatry in 2003.
“I feel privileged to be a part of this, because I think—and most people involved in TMS believe—that this is just the beginning.”
The treatment, he said, has been proven effective in treating a variety of other conditions as well, such as obsessive-compulsive disorder (OCD), Autism, dementia, PTSD and traumatic brain injury. And at military institutions, including the VA, where it is already in use in psychiatry.
“And that is exciting because these are all conditions where we have very little options,” he said.
As with any new treatment, there are those both in and out of the medical community who still need convincing.
“I respect them,” Dr. Sheth said. “I don’t call them cynics, because we have to be able to have a healthy conversation with everything we do in healthcare. It also keeps us humble and grounded, in that this is not a cure. This doesn’t mean that someone gets treatment, that they will never need any more treatment the rest of their lives.”
According to Achieve TMS’s statistics, the majority of people—more than half—do well until after a year, and there is a small percentage of people who come back within and year and say their symptoms have returned.
“But the thing is, most people are more aware, and they are more hopeful that they can get better,” Dr. Sheth said. “Because one of the things that happens with depression, after maybe two or five years, is that most people develop this sense of hopelessness; They say, ‘Okay, well, I take this medication, and I’m doing a little bit better, but I’m never going to be completely better.’ And when they get TMS, and when they get remission, they think, ‘Okay, well there is life beyond this. There is hope to this tunnel.’”
—Mick Rhodes
mickrhodes@claremont-courier.com










0 Comments