L.A. County new virus cases skyrocket to serious numbers
by Steven Felschundneff | steven@claremont-courier.com
On Monday, Los Angeles County Department of Public Health Director Barbara Ferrer delivered a stark warning to county residents, “Assume that this deadly, invisible virus is everywhere looking for a willing host.”
Speaking at the first joint-powers coronavirus news conference of the new year, Ms. Ferrer outlined in great detail how the actions of some residents who gathered or traveled during Thanksgiving—and now the holiday week—were driving an unprecedented spike in new COVID-19 cases, which inevitably leads to increased hospitalizations and tragically, deaths.
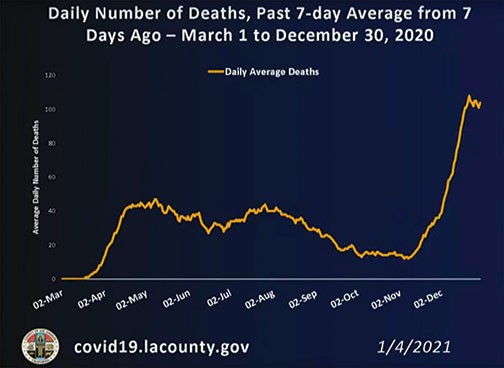
On Wednesday those words certainly seemed to hold truth as the county reported 258 deaths and a remarkable 8,023 people currently hospitalized with COVID-19 symptoms. For weeks local hospitals have been above capacity and the situation will only get worse as the people who gathered during Christmas and for New Year’s Eve parties become sick.
“Given the current state of the pandemic in Los Angeles County, the worst is almost certainly still ahead of us,” Director of the Los Angeles County Department of Health Services Dr. Christina Ghaly said. “We do not believe that we are yet seeing the effects of the holiday. This is unfortunately in our future.”
Speaking about the four Department of Health Services hospitals, Dr. Ghaly said over half of beds are filled with COVID-19 positive patients, and three quarters of people receiving critical care services in the intensive care units are there because of COVID-19.
The community spread is so acute currently that one in every five people who test for the coronavirus receive a positive result. It took nine and half months to reach 400,000 cumulative cases in the county, but infections have more than doubled since December 1, surpassing 800,000.
“The rate of new cases this month is translating into a disastrous increase in the number of people with severe COVID-19 symptoms being sent to our local hospitals and, tragically, we are now seeing more than 200 deaths a day. People who were otherwise leading healthy, productive lives are now passing away because of a chance encounter with the COVID-19 virus. This only ends when we each make the right decisions to protect each other,” public health officials said in a news release.
As of Wednesday, public health has identified 852,165 cumulative cases of COVID-19 across all areas of L.A. County and 11,328 deaths. There were 11,841 new cases reported Wednesday.

Here in Claremont there have been 42 new infections in the last two days, for a cumulative total of 1,587. Tragically, four more Claremont residents have died this week, bringing the total to 29. Public health is reporting 395 cases in the past two weeks, which provides a rough indication of how many people here are currently ill.
Health officials issued a citation for lack of compliance with the health order to B. C. Café on December 26. Several other Claremont restaurants were given similar citations earlier in December.
With all of the troubling news about the coronavirus, there is a glimmer of hope as tens of thousands of county residents have received the vaccine, with more doses on the way. Currently the county is in phase 1A of the vaccination program, administering the inoculation mainly to healthcare workers at the greatest risk of exposure. This week, the county opened 18 vaccination sites where frontline healthcare workers can get vaccinated on an appointment basis.
As of Monday, a total of 185,250 doses of the Pfizer vaccine have been received and 100,556 have been administered to frontline healthcare workers at acute care hospitals. About 1,600 healthcare workers who were among the first to receive the vaccine in mid-December have been received the second dose and are fully vaccinated.
The county has received 166,300 doses of the Moderna vaccine as of Monday, of which 31,915 have been administered to staff and residents at skilled nursing facilities as well as emergency medical technicians, paramedics, and healthcare workers in clinics.
Currently, appointments at the 18 vaccination sites are being accepted only for healthcare workers at high or medium risk of COVID-19 exposure who work in specific settings. These settings include: Acute care hospitals; federally qualified health centers; home healthcare organizations; infusion and oncology centers; intermediate care facilities; residential or inpatient substance abuse and mental health facilities; urgent care clinics; primary care clinics, rural health centers and correctional facility clinics, according to public health.
“We hope to begin vaccinating priority groups in Phase 1B in early February, assuming adequate supply of vaccine. The state has identified two tiers in Phase 1B. Tier 1 in Phase 1B includes: individuals 75 and older, and those at risk of exposure in education, childcare, emergency services and food and agriculture; Tier 2 in Phase 1B includes persons between the ages of 65 and 74, those at risk of exposure if you work in transportation and logistics; in industrial, commercial and residential and sheltering facilities and services; in critical manufacturing; and congregate settings with outbreak risk including homeless and incarcerated. For Phase 1B we are planning for eligible priority groups to be able to go to registered primary care providers, pharmacy partners, or community vaccination sites. And we hope we are able to move to Phase 1C, assuming adequate supply of vaccine, by late March, early April,” county officials said in a statement.
Supervisor Hilda Solis said during Monday’s news conference that the county has adopted a policy to provide priority access to the vaccine for people hardest hit by the pandemic including Latino and Black communities.
She cited the hospitalization rate for Latinos, which at 80 per 100,000 residents is three time that of white residents as an example of the need to prioritize inoculation in these communities. Blacks have a hospitalization rate of 57 per 100,000.
“These figure make clear that we need equitable distribution of the vaccine in disadvantaged neighborhoods in part because many of theses areas are comprised of essential workers,” Supervisor Solis said.
These communities include East Los Angeles, Boyle Heights, San Gabriel Valley and Pomona.









0 Comments